What is a Vesicovaginal Fistula
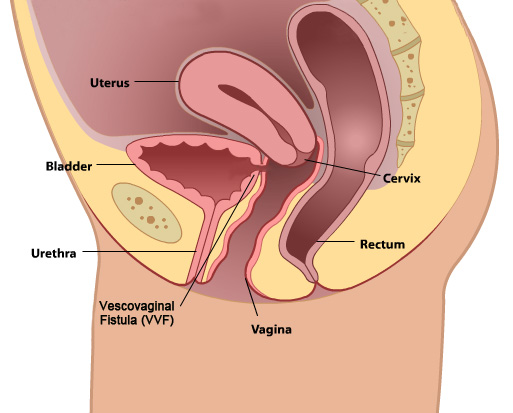
A vesicovaginal fistula is an abnormal connection between the bladder and the vagina, which subsequently continuously drains urine. Certainly there are medical complications and sequalae from a fistula, but perhaps even more devastating are the emotional and social consequences of continuous urine leakage, leading to significant social and functional limitations. The majority of vesicovaginal fistulas in developed countries are the result of gynecologic surgery, most commonly hysterectomy. Inadvertent bladder injury during surgery accounts for a large proportion of future vesicovaginal fistulae. However, the presence of a bladder injury does not mean a fistula will necessarily develop. Several other factors play a role in the formation of a fistulous tract. Other types of urinary fistulas can also form, including urethrovaginal (urethra to vagina) or ureterovaginal (ureter to vagina) fistulas.
Symptoms of a Vesicovaginal Fistula
Continuous urinary leakage is the most common presentation of a vesicovaginal fistula. In some, this is first noticed as an increase in vaginal discharge or drainage. Most patients will present one to four weeks after hysterectomy. A very small defect may not produce continuous leakage and intermittent urine may be noticed.
Evaluation of a Vesicovaginal Fistula
When a patient presents with concerns for a vesicovaginal fistula, our practice typically will perform an office cystoscopy (small camera that looks inside the bladder) to assess the location and proximity of the fistula to the ureteral openings in the bladder. The ureters carry the urine from the kidney to the bladder; if the fistula is very close to the ureter, additional surgical planning and treatment may be required.
Most experienced surgeons will utilize a transvaginal approach for repair of a vesicovaginal fistula and reserve the abdominal route for complicated fistulas or cases that have failed prior surgical intervention.
Surgical Planning for a Vesicovaginal Fistula
Repair of a vesicovaginal fistula is a highly technical skill and should be performed by a surgeon with expertise and experience in fistula repair. The greatest opportunity for cure lies in the first surgeon’s hands. With each failed repair, the complexity to achieving success becomes more challenging. Our practice is experienced in performing surgical fistula repair, and Dr. Veronikis has repaired over a hundred cases of urogenital fistula.
The timing for surgical repair can vary based upon the etiology of the fistula and how long it has been since the inciting event (hysterectomy). Sometimes a delay to allow the acute inflammation to heal is recommended to permit the return of healthy tissue prior to surgery.
Surgical Repair of a Vesicovaginal Fistula
In our surgical philosophy of fistula repair, there two important tenets of successful closure of the defect:
- Tension-free repair to allow proper healing
- Closure of the high pressure organ (bladder)
These are both critical whether the repair is completed vaginally or abdominally although our primary modality in closing most fistulas is vaginally. Some patients have a fistula secondary to mesh that has eroded into the bladder and the vagina; these patients will need removal of the mesh and repair of the fistula to achieve continence.
Following the surgical repair, an indwelling urinary catheter will be necessary to continuously drain the bladder during the first seven to ten days. After this time, our practice performs a post-op office cystoscopy to examine the surgical site. If the healing appears to be appropriate, the catheter is removed at this time.
